Knowledge you can build upon
Improving Patient Care in Hospitals, Creating Team Behavior
By Beatrice J. Kalisch & Susanne Begeny
Introduction
If you are hospitalized your interest is likely to center on getting well. The way you will get well is to receive the medicine, therapy, and care appropriate to your condition. The delivery of a major portion of the attention you require will be in the hands of the patient care staff.
" ...teams come in gradations."
It would be nice to believe that the people taking care of you were functioning as a team. You would want the patient care staff focusing on a common objective—your health. You would want each member of the staff prepared to do what is needed to care for you regardless of their "job." Unfortunately, you are likely to be disappointed. Patient care staffs in hospitals typically do not function as "teams."
The lack of teamwork in patient care is not due to the people. The only reason that hospitals work as well as they do is the dedication of their professional staffs. The problem is that groups are not seen as instruments for the delivery of health care. Rather, the focus centers on individuals. For example, the ratio of Registered Nurses (RN) per patient is watched closely. The fact that the RN may have to manage a group of people who may not know each other is ignored. In other words, the problem is structural and not personal.
The Concept of "Team"
A "team" is a group of people working in a coordinated manner. There are two absolute requirements for teams (Salton, 2004): common purpose (e.g., aim, goal, objective, etc.) and common destiny (i.e., accountability for any and all results produced by the team). Common purpose sets the direction. Without it, people can be "pulling the wagon" in all directions at the same time. A lot of effort is spent but nothing moves. Common destiny provides the motive for "pulling the wagon" in a common direction. Without a stake in the outcome, there is no reason to try to "pull the wagon" in any direction.
"...nursing care teams offers hospitals an opportunity."
Like most things, teams come in gradations. At one end of the scale might be a hospital's Volunteer Services Group. The common purpose is a generalized desire to help people in distress. The common destiny is the satisfaction associated with participating in a group that is doing something worthwhile. Team behavior may be present but will probably not be strong.
At the other end of the scale might be a children's neurosurgical team. Here the purpose is explicit and immediate—remove the tumor without causing damage. Common destiny is equally vivid. A success or failure on the part of any team member instantly reverberates to all others. Team behavior is likely to be strong and highly visible.
Nursing Care Factors
Common purpose and common destiny underlie all team behavior. They give the direction and motive for action. However, the processes, practices, and procedures of a hospital effect the ability to actually fulfill the purpose and create the desired destiny.
Organizational Engineering (Salton 1996, 2000) offers a lens to see hospital practices in terms of their effect on teamwork. These factors form a network or system of influences. Each effects the other. Addressing any one may or may not improve team performance. Addressing them all will always move a group toward increasing team behavior.
These factors include:
Team size:
Choosing the wrong team size can make teamwork impossible.
Coordination:
Predictability is the core of any form of coordinated action.
Stability:
Too much variability ensures inferior performance.
Common Purpose:
This is often taken as a given by hospitals. It is not.
Common Destiny:
This is a requirement for team behavior.
Physical Environment:
The distribution of people in space matters.
The factors governing team behavior are entwined. However, understanding the operation of each factor requires that they be considered separately. Team size is perhaps one of the more obvious and important aspects of teams.
1. Team Size
Size is a critical factor of the ability of a group of people to function as a team. The reason for this primacy is the concept of a transaction channel (Salton, 2004). This is a relationship under which each party to a transaction must consider the proactive and reactive actions of another. This channel can involve communication, influence and expectations. Maintaining this type of relationship is not free. Both parties must participate to maintain the channel. There is a cost to all involved.
Consider Figure 1 to be a group taking care of a patient. If additional help is required to care for a patient, such as ambulating him, another nurse would need to be added.
Figure 1
Transaction Channels
Three person group-3 channels
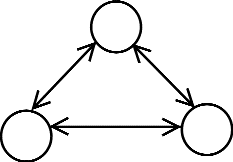
Figure 2 shows the effect of this action. The number of channels has increased from 3 to 6. A 33% increase in team size has doubled the number of channels that each team member must consider.
Figure 2
Transaction Channels
Four person group-6 channels
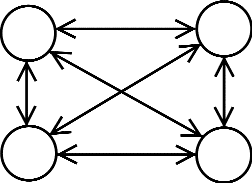
The geometric progression continues as team size increases. Figure 3 shows how quickly transaction channels increase with additional people. Each channel can be thought of as an overhead burden imposed by team size.
Figure 3
Group Size vs. Transaction Channels
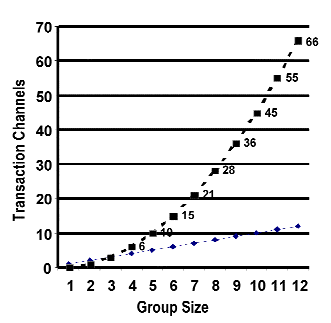
Research literature sets a normative team size of 5 to 12 people. The South Florida Water Management District reports an average group size of 6 (Vann, 1999). President Clinton's National Performance Review found an average federal group size of 8 people (Friel, 2001). The National Guard manual implies average group size of about 9 (U.S. Army Field Artillery Center, 2003). Pierce County, WA reported an average group size of 7 while Portland, OR had a mean group size of 8 people (Peat Marwick LLP, 1998).
Professional Communications, Inc. has been collecting data on the teams analyzed using its proprietary programs. At the time of this article, its database contained 2,267 teams (Nelson, 2005).
The database is national in scope and covers a spectrum ranging from drilling oil wells to developing new medical devices.
Figure 4 Group Size Actual Experience n=2,267 teams
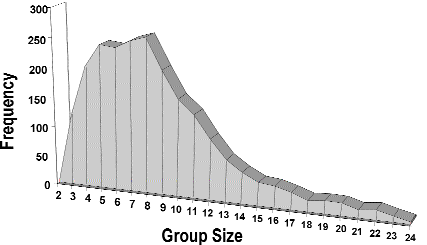
Figure 4 shows that the most frequent team size encountered is between 5 and 8 people. The average, which takes into account very large teams, is about 9 people. It is reasonable to assume that real firms functioning in the world find teams of between 5 and 9 people to be operationally optimal.
Even CEO teams seem to fall in the operational optimality range. In 1999, the average CEO (178 firms) had 6.7 direct reports, an implied group size of 8 people (Rajan and Wulf, 2003). Ernst & Young (2003) provides international confirmation of this estimate by citing group sizes of 5 to 8 for CEOs and general managers among 36 major firms. Team size seems to be governed by transaction channels regardless of the level of the team being considered.
Patient care teams are usually led by RNs and can include Licensed Practical Nurses (LPN), Nurse Aides (NA), contingency/float nurses, agency/traveler nurses, and unit secretaries. These are the people who deliver and support the nursing care for which a hospital is praised or condemned.
Nursing teams appear to be formed capriciously. Sometimes a single team is created for an entire ward of 100 beds. At other times patient care units are segmented into pods. The co-author (Kalisch) has seen teams as large as 90 people. The choice of size seems to be governed by everything except the organizational implications for patient care.
2. Coordination
Team size is important because it effects the ability of people to anticipate each other (Salton, 2005). For example, a nurse may be especially skilled at starting IVs or preparing a patient to take care of himself after knee surgery. If this strength is unknown, it cannot be drawn upon by others. In the absence of familiarity, the only thing that can be depended on are the nurse's basic skills. Basic skills are just that, basic. Excellence is seldom achieved by exclusive reliance on basic abilities.
The authors investigated the degree of familiarity among sixteen nurses working on a medical-surgical unit (Kalisch and Begeny, in press). They were selected at random and tracked for one month. The analysis calculated how many different individuals the sixteen nurses interacted with. This includes the people they worked with on their shift as well as staff they took or gave reports to as shifts changed. Excluded were non-unit staff interactions such as physicians, support and unit staff, as well as visitors. Effectively, each unique person represented a transaction channel in which parties try to anticipate and complement the other.
The analysis showed that each of the 16 nurses worked with an average of 36 different staff members over the month. The nurse with the largest number of interactions worked with 48 different people. The nurse with the fewest number, worked with 29 different people. The remaining nurses averaged in the mid-thirties. The difference between the high number and low number was based on: (1) the length of shift, and (2) whether the nurse was full-time or part-time/contingent staff.
An 8-hour day shift nurse can illustrate the effect of the shift length. On beginning her shift she receives a report from the midnight shift. This represents one cluster of interactions. She then works with the other staff on her shift, a second cluster of interactions. Her final cluster are individuals she gives reports to as she exits her shift.
The 12-hour shift nurse had the same interactions as the 8-hour nurse plus an additional two. One of the added clusters are the new nurses she works with for part of her 12 hours. The other cluster is the nurses who receive her patients after she has completed her final 4 hours. The larger number of interactions on the 12-hour shift means that these nurses have to manage more interactions. Coordination be-comes more difficult and team functioning declines.
The lower ends of the interaction scale are the part-time or contingent nurses. These nurses are seen only a few times. Short working hours do not provide as many interaction opportunities. This lower level of exposure means less familiarity. In other words, they interacted with fewer people but less often. Familiarity did not have time to build.
The above analysis does not describe teams, it only considers the different people with whom the nurse may form a team with. The research was extended to look at the different individuals that actually appeared in the sampled nurses’ work group. On average, three different people showed up on the work group each time a sampled nurse reported for a shift. It is reasonable to expect that a lack of familiarity with the work practices of these people will cause deterioration in team performance.
The research also showed an individual variation. One nurse worked with six different individuals. This was about double the overall average of three new staff members. She also worked the least number of shifts in the group studied. Yet she interacted with more new people every time she worked. This means that she had less opportunity to become familiar with her co-workers and they with her. This illustrates an effect of part-time nurses on familiarity and, thus, on coordination capacity.
This analysis illustrates but understates the challenge. The sampled nurses also worked with unit secretaries and nurse managers as well as a variety of specialty functions (therapists, social workers, etc.). These unconsidered transaction channels compound the challenges nursing care teams face as they try to provide efficient, effective care.
3. Stability
The stability of staff directly impacts familiarity and ,thus, team effectiveness. Adams & Bond (Adams and Bond, 2003) showed that where instability was high, the standards of professional nursing practice were seen to be low. While other factors also contributed (e.g., commitment, skill levels, etc.), the lack of familiarity undoubtedly had a strong influence.
One source of instability is agency and traveler staffing. These people work for firms who supply hospitals with needed people on a demand basis. While these people carry the same professional qualifications as permanent staff, they are typically seen as an inferior resource (Adams & Bond, 2003 p. 294). Some portion of this verdict is due to familiarity. The agency nurses do not know the team's practices and preferences well enough to effortlessly integrate their behavior. The inferior performance is attributed to the resource rather than to the structure within which they work.
The literature in the field, the data from this research, and common sense all confirm the instability of nursing care teams. Nurses work different days of the week, different shifts and in varying amounts. They work with nurses "floated" in from different units. Agency staffs appear and disappear. Part-time staff may work only a few hours a week and even then not consistently. The mixing of 8 and 12 hour shifts incresases instability. Throughout this process patients are entering or leaving, changing the work demands on the unstable teams.
It is not surprising that patient care appears to be in a crisis. What is surprising is that it works as well as it does. It is a testimony to the professional dedication of nurses that hospitals function as well as they do.
4. Common Purpose
The common purpose of nursing care seems obvious—take care of the patient. However, what "care" involves may not be held in common. For example, one nurse may view her charter as the patient's well-being on her shift. Another may see the discharge of the patient in good healthas the goal. Some nurses view their purpose as involving all of the people who work with them. Others may focus only on their own individual performance.
Not only might common purpose be obscure within a team, it can also vary between teams. One shift may take a narrow view and see their purpose as getting through the shift. Another might see the overall well-being of the patient during their entire hospitalization as their charter.
A patient experiencing an ambiguous common purpose is likely to see a variation in the care. At best, their likely judgment is that hospital quality is uneven. At worst, quality will be seen as sorely lacking. Poorly defined common purpose ensures that teams will behave in a less than fully coordinated fashion. The hospital and nursing executives who neglect to define a clear and compelling common purpose can expect to reap mediocrity, at best, as a reward.
5. Common Destiny
Common destiny is the motive for pursuing common purpose. It is what causes a team member to "feel" a share in the outcome of a team effort. This "feeling" is there whether or not they participated in the specific activity that generated it.
Team size is a major influence on whether a person sees their interest as being entwined with that of the group. For example, a member of a 50 to 80 person "team" may have difficulty in seeing a dissatisfied patient as reflecting on them. Responsibility is simply too diffuse and personal contribution too small as a proportion of the total.
The reward structure also effects the perception of common destiny. Groups might see their interdependency better if rewards (e.g., pay, bonus, days off, etc.) were allocated to groups rather than individuals. However, large team size, instability, low familiarity, and a weak vision of common purpose would render this option ineffective as a "stand alone" tool. It has a role but the other factors must be addressed for it to have a material effect.
6. Physical Environment
Another influence on teamwork is geography. The layout of the unit can effect the likelihood of teamwork. For example, a nurse working on a unit with two hallways and no line of sight will find it difficult to coordinate her actions with those of her team. If you do not know when help is needed, you are unlikely to give it.
Physical distance also effects teamwork. Long distances mask the opportunity for cooperation and can increase the cost of providing it. It causes division of labor to dominate over teamwork. Synergistic cooperation, one foundation of team behavior, is minimized.
The "take home" of this observation is that hospitals should consider where the team is working as well as its size, stability, familiarity, purpose, and destiny. Physical conditions can and do matter.
Recommendations for Action
Increasing patient care teamwork will improve the quality of nursing as well as the functioning of a hospital. It need not cost more. It only requires that hospitals engineer the structure of their organized groups. The following recommendations are not rocket science. They follow directly from the transparent analysis that preceded them.
1. Team Size
Smaller teams reduce the number of interaction channels. The senior author personally experienced this effect at a Michigan hospital. Smaller teams were created by dividing a 40 bed medical unit into four ten-bed units. Staff agreed to work for one year on one of these ten bed units. This made it possible to work with the same people both during the shift and for the shift handoffs.
The initiative reduced the number of different people the staff had to work with by 75%. Instead of interacting with 60 different staff members, they only worked with 15. The results were rewarding. The teams adopted names. This indicated that the teams were being thought of as "things" independent of the specific people who comprised them. Patient satisfaction increased markedly. Patients even wrote complementary letters to the local newspaper. They said that if they needed to be readmitted, they wanted to be in the wing serviced by the team that had cared for them in their recent stay. Staff satisfaction also increased.
2. Scheduling
Consistent staffing reduces the number of different people a nurse must work with. This means that familiarity increases and the probability of team behavior improves. Consistent staffing also enhances patient safety, quality of care, and patient satisfaction. If nurses worked set schedules, a patient would better know what to expect and how to get what he/she wants. Consistency also gives enough time for a degree of rapport to be established. This is likely to improve patient outcomes as well as the patient's judgment of hospital quality.
Patient assignments and work team participation can never be totally consistent. However, consistent schedules improve the odds of team behavior. It is the natural outcome of people getting to better know each other's strengths, vulnerabilities, and preferences.
3. Shifts
Another issue effecting team behavior is the mixture of 8 and 12 hour shifts. If 8 and 12 hour shifts were randomly distributed, patients would be redistributed every 4 hours as one nurse left in the middle of another's shift. While this kind of universal reallocation seldom occurs in the real world, it really does occur every time 12 and 8 hour shifts are mixed. When it does, the result is not good for the patient nor the nursing team.
The obvious solution is to try to create consistent 8 or 12 hour shifts. If this is impossible a structural adjustment might be attempted. For example, staff members desiring to work 8 hours might be bundled together as a team. Workloads might be designed so that these people hand off to another 8-hour team. This strategy might create cohesive units around preferred working hours.
4. Incentives
Four categories of rewards are applicable to nursing. Financial rewards (e.g., raises, bonuses) are expensive and can lose value if not seen as equitable. Status symbols (e.g., plaques) are cheap but lose value if they are seen as manipulative. Social rewards (e.g., recognition) are inexpensive but are not durable. Opportunity (e.g., promotion) is a strong motivator but is limited by the number of openings available.
Aligning a mix of rewards with desired behaviors is the job of management. There is no "silver bullet." Effective reward systems will be a mixture of all available tools. Whatever the mix, the key is to reward the right behaviors. If teamwork is the goal, groups should be rewarded and not individuals. Badly aligned rewards will produce results. They will just be the wrong ones.
The right mix of rewards and the behaviors to be rewarded will be local. What works in Chicago may not work in Santa Fe. An effective system for a 300 bed general care hospital may not be right for an 800 bed research oriented medical center. Management should be prepared to "wrestle" with this issue. It is worth the effort.
5. Proximity
Physical proximity matters. Close proximity lowers the cost of using transaction channels. It improves the odds of recognizing opportunities for team cooperation. It can become a source of team pride and even a matter of team identity (e.g., the 3-South Team). Hospitals have long recognized physical geography as a component of care (e.g., proximity of the MRI to the emergency room). They need only extend the concept to the functioning of the rest of the hospital.
Conclusion
The creation of nursing care teams offers hospitals an opportunity to improve patient care, increase efficiency and enhance staff effectiveness. This can be done without investing millions in capital improvements. All that is needed is to align practices, processes, and procedures in a way that allows nursing and other patient care teams to form.
Aligning all of the factors (e.g., team size, stability, consistency, etc.) is not a "cookbook" process. Local circumstances must be considered. However, this article has identified the major factors. Their effect on each other has been cited. Working out the exact "formula" for a particular hospital will be an iterative process involving all of the stakeholders. The outcome, however, will pay large dividends to all involved.
AUTHORS
Dr. Beatrice Kalisch is the Titus Distinguished Professor and Division Director of Nursing Systems at the University of Michigan in Ann Arbor. In addition to her University work, she also has her own firm which specializes in consultation with health care organizations in the areas of nursing strategic planning, innovation, change, patient care systems and healthcare operations. She holds a Baccalaureate Degree in Nursing from the University of Nebraska and a Masters Degree in Nursing from the University of Maryland, Baltimore. She also earned a doctoral degree from the University of Maryland, College Park.
Dr. Kalisch has authored several books, published over 80 articles and has made over 500 presentations throughout the world. She is listed in numerous bibliographies such as Who's Who in America and Who's Who of American Women. Dr. Kalisch is a fellow in the American Academy of Nursing. She serves as a member as well as leader in numerous local, state and national advisory committees addressing health policy and nursing issues. Dr. Kalisch has been the recipient of many awards including distinguished alumnae at both the University of Maryland and the University of Nebraska.
Suzanne Begeny received her Bachelors of Science in Nursing and Bachelors of Art in psychology from the University of Michigan in 2002. Her Master's in Nursing Business and Health Systems was obtained in 2004 from the University of Michigan School of Nursing. Currently, she is in the doctoral program at the University of Michigan and a research associate for Dr. Beatrice Kalisch. Her area of focus is health care policy, political participation and how it relates to the nursing profession. Other research interests include the image of the nurse, organizational change, and recruitment and retention strategies.
Beatrice Kalisch:
400 N. Ingalls, Room 4170, School of Nursing, University of Michigan, Ann Arbor, MI 48109, 734-936-3683, bookmana@aol.com
Suzanne M. Begeny:
400 N. Ingalls, Room 4154, School of Nursing, University of Michigan, Ann Arbor, MI 48109, 734-657-2097, sbegeny@umich.edu
BIBLOGRAPY
Adams A, Bond S. (2003). Staffing in acute hospital wards: part 2. Relationships between grade mix, staff stability and features of ward organizational environment. Journal of Nursing Management. 11, 293-298.
Adams A, Bond S. (2003).Nursing organisation in acute care: the development of scales. Report no. 71. Centre for Health Services Research, University of Newcastle upon Tyne, Newcastle upon Tyne. As cited in Adams A, Bond S. (2003) Staffing in acute hospital wards: part 2. Relationships between grade mix, staff stability and features of ward organizational environment. Journal of Nursing Management. 11,294.
Cusumano MA. (1997)..How Microsoft makes large teams work like small teams. Sloan Management Review. 39(1)9-20.
Ernst & Young, 2003. Human Resources Benchmarking Report: Sultanate of Oman 2003. Ernst & Young Human Capital Services. Accessed January 23, 2005.
http://www.ey.com/global/download.nsf/...
Friel, Brian, 2001. Drop in projected retirements puts Bush management cuts at risk. GovExec.com.
http://www.govexec.com/dailyfed/0501/052201b1.htm
Kalisch, Beatrice J. 2005. Teamwork Issues on Patient Care Units. University of Michigan, School of Nursing. Unpublished report.
Kalisch, Beatrice J. and Begeny, Suzanne. Nursing Unit Teamwork: Why Is It So Difficult and What Can Be Done About It?, Journal of Nursing Administration, in press.
Katzenbach ,,Jon R. and Smith, Douglas K. The Wisdom of Teams. Boston: Harvard Business School Press, 1993.
Nelson, Shannon (2005). VP & Chief Operating Officer of Professional Communications, Private research and counsel, January 2005.
Peat Marwick LLP (1998), Performance Audit of Perce County, Washington. Volume II. Technical Appendix. http://64.233.161.104/search?...
Raghuram G. Rajan and Julie Wulf (2003). The Flattening Firm: Evidence from Panel Data on the Changing Nature of Corporate Hierarchies.
Management Seminar, Columbia University, September, 2003. http://64.233.161.104/search?...
Salton, Gary J. (1996). Organizational Engineering. Ann Arbor, MI: Professional Communication Inc.
Salton, Gary J., 2000). The Manager's Guide to Organizational Engineering. Amherst, MA: HRD Press.
Salton, Gary J., 2004. Organizational Engineering Seminar, Ann Arbor, MI. October 2004.
Salton, Gary J., 2005. Chief: Research and Development and CEO, Professional Communications, Inc. January, 2005. Personal Conversation.
Vann, Allan (1999). An Interim Study of Span of Control. Office of Inspector General. South Florida Water Management District. http://www.sfwmd.gov/org/ing/SpanCtrl.pdf
U.S. Army Field Artillery Center,2003. Field Artillery Proponent Briefing 13; Career Management Field. Accessed January 23, 2005.
(C) 2005, Organizational Engineering Institute. All rights reserved
Organizational Engineering Institute
101 Nickels Arcade
Ann Arbor, MI 48104
Phone: 734-662-0052
Fax: 734-662-0838
E-Mail: OEInstitute@aol.com
ISSN: 1531-0566
Printed in the United States of America